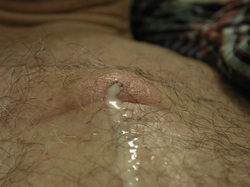
 The cloudy drainage from this implanted port presented several weeks after implantation. It was inserted via the left subclavian vein without incident during the surgical procedure. The incision had healed and sutures had been removed. When accessed with a 20-gauge port access needle, this cloudy fluid began to leak from the puncture site. More exudate continued after removal of the needle. So what could this be? A serious port pocket infection? Extravasation of the previously infused fluid? This is chyle – a combination of lymph fluid and free fatty acid from the small intestines. The fluid passes through the lymph system where it enters the bloodstream through the thoracic duct located at or near the junction of the left internal jugular and subclavian veins. A smaller thoracic duct can also be found on the right side. During insertion of any central venous catheter (including PICCs), these thoracic ducts can be damaged, causing the chyle to leak into the pleural space or externally. In this case, the chyle tracked along the catheter and accumulated in the port pocket. Accessing the port caused the chyle to leak from the puncture site. Although rare, it is important to be aware of this complication from CVADs. Several articles can be downloaded about this complication. Click these links to learn more. Chylothorax - A Complication Of Peripherally Inserted Central Catheters Thoracic Duct Cannulation During Central Venous Catheterization: A case Report Iatrogenic chylothorax due to pleural cavity extravasation of total parenteral nutrition in two adults receiving nutrition through a peripherally inserted central catheter. 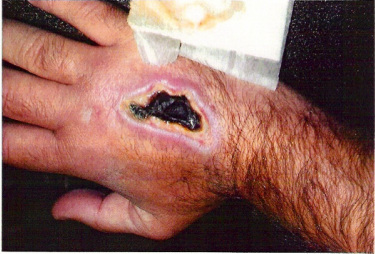 Necrotic ulcer 5 weeks after promethazine extravasation Necrotic ulcer 5 weeks after promethazine extravasation I am closing yet another case involving extravasation of promethazine. When will these cases end? Although the Institute for Safe Medication Practices (ISMP) issued warnings and recommendations about I.V. promethazine in 2006, many hospitals have not addressed this issue. The ISMP includes promethazine on their List of High-Alert Medications in Acute Care Settings. Click here to download this list http://www.ismp.org/tools/highalertmedications.pdf Read case reports of what promethazine can do to subcutaneous tissue here. http://www.ismp.org/Newsletters/nursing/Issues/NurseAdviseERR200608.pdf A completely patent I.V. site is a mandate for promethazine. The most important things to assess include:
Think carefully about how you and your colleagues give this drug by the I.V. route. ISMP recommends dilution, yet the manufacturer’s instructions state it can be given undiluted. I strongly recommend dilution in a 10 mL syringe and pushing slowly while aspirating for a blood return every 2-3 mLs. Dilution in a minibag and giving by piggyback is not a good practice, in my opinion, because the nurse will leave while this is infusing and there is no constant monitoring of the site and frequent checks for blood return. In addition, there must be fluids infusing through the site while you are injecting promethazine to provide additional fluids to flush the vein. A small gauge catheter in the largest vein possible will increase the blood flow around the catheter but infusing fluids also are recommended. Once promethazine has entered the tissue, there are very few, if any, effective treatments. Therefore, prevention of extravasation is crucial. So, take plenty of time to assess this I.V. catheter and vein for complete patency. As will all drugs, the person giving the medication is responsible for doing the procedure, but we are also held accountable for the outcome of our actions. If there is no prescription for infusing fluids, ask for the order. Suggest other medications instead of promethazine. Alternatively, suggest another route of administration if promethazine is the best drug for your patient. Lawsuits with this drug continue including outcomes of CRPS, necrotic ulcer with or without surgical debridement, and amputation. Most lawsuits will end in a settlement out of court, which always means a private agreement. This is the reason that the number of actual cases and the dollar amount of the settlements are unknown. A nurse with knowledge about the risk with promethazine, and the correct administration methods, along with the skills for an in-depth I.V. site assessment can prevent these problems, protect your patient from the devastating injuries, and protect yourself and facility from a lawsuit. Caption for picture |
Author: Lynn HadawayLynn Hadaway is an international thought leader in infusion therapy and vascular access, having been in this practice for more than 40 years. Her experience comes from hospital-based infusion teams, device manufacturers, and continuing education services. Her journal and textbook publications are extensive. She also maintains board certification in infusion nursing (CRNI) and nursing professional development (RN-BC). Categories
Archives
May 2019
|
Copyright © 2020 Lynn Hadaway Associates, Inc. | P.O. Box 10, Milner, GA 30257 | 770-358-7861


 RSS Feed
RSS Feed